Malaria is a deadly disease, which spreads to humans through the bite of infected Anopheles mosquitoes. The African region carries a disproportionately high share of the global burden of malaria, accounting for 95% of global cases. In Tanzania, where we live and work, the entire population is considered at risk of the disease, making it one of the most pressing health challenges in the country. As one of 11 African countries classified as “high burden”, Tanzania faces persistent transmission hotspots, particularly in the lake and coastal zones.

Scientists at Ifakara Health Institute in Tanzania are working towards innovative new vector control tools as part of the Transmission Zero partnership. Photograph: Malaria No More UK/Jordi Mat
Co-led by scientists at the Ifakara Health Institute (IHI), the Tanzania National Institute for Medical Research, the Swiss Tropical and Public Health Institute (Swiss-TPH) and Imperial College London, the Transmission Zero international research programme is working to develop innovative genetic tools aimed at reducing malaria transmission by targeting its source: the mosquitoes that transmit the disease.
Our work at the Ifakara Health Institute
At Transmission Zero, our work represents a shift in the development of innovative tools for malaria control — from a model in which the design and development of new approaches have been traditionally carried out outside of the African region, to one that is led and owned by African institutions. Through long-term collaboration and knowledge exchange between partner institutions, a new generation of Tanzanian scientists has been trained in molecular biology, vector genetics, and biosafety, ensuring that scientific discovery and leadership remain firmly rooted in the African region. At the Ifakara Health Institute and the National Institute of Medical Research we have taken the lead in developing and testing our technologies under the oversight of institutional and national ethical and regulatory bodies, while our Imperial College partners have supported capacity building and advanced training.
This leadership has already delivered historic results. In 2023, we achieved a major milestone by successfully developing the first genetically modified mosquito in Africa. Working under laboratory containment, we introduced naturally occurring antimalarial molecules into local mosquito populations. The results were groundbreaking: we were able to show that our technology is able to effectively block the development of the malaria parasite, creating a powerful barrier to transmission of the disease.
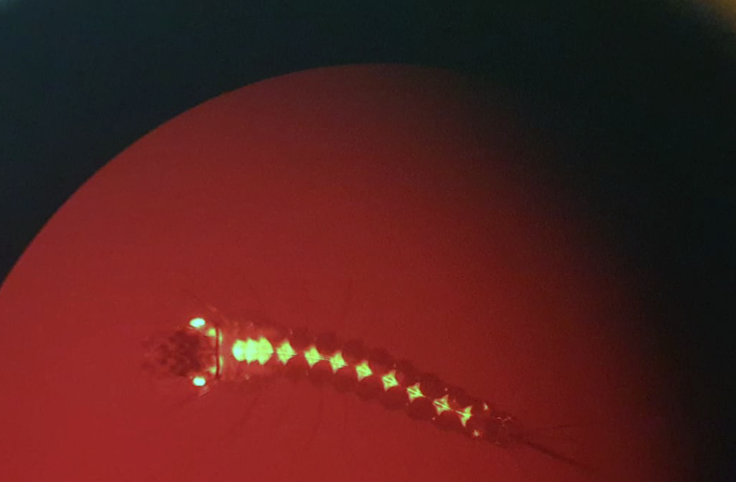
A transgenic mosquito larva through the lens of a microscope at the Ifakara Health Institute. Photograph: Ifakara Health Institute
The research was conducted in a state-of-the-art Modular Portable Laboratory and Containment Level 3 insectary facility (MPL/CL3) built specifically for this research at the IHI campus. This facility, designed to meet high biosafety standards, enables local researchers to lead genetic engineering efforts and ensures that the technology is developed responsibly and transparently within Tanzania.
This is the first time a genetically modified, gene drive-compatible mosquito strain has been developed in Africa, by African scientists, targeting malaria parasites circulating in local communities. We are proud to be driving innovation locally, using cutting-edge tools to address one of our continent’s most pressing health challenges. – Dr. Dickson Wilson Lwetoijera, Programme Director at IHI
Building on this progress, our next steps focus on ensuring that this innovation is safe, effective, and ready for potential testing in the field. We are advancing comprehensive risk assessments, engaging closely with regulators, and continuing community consultation to ensure transparency and trust.
Innovation rooted in partnership
While leadership is local, our success is also built on strong international partnerships. Imperial College London serves as the programme’s primary grant recipient and scientific co-lead, working alongside IHI, NIMR, and the Swiss TPH. This collaborative model is paramount to ensure sustainable capacity strengthening through infrastructure development, and knowledge and technology outputs.
Our partnership model is deliberately equitable. Research questions are co-developed, decision-making is shared, and expertise flows in both directions. Imperial College contributes longstanding experience in the development of gene drive technologies, molecular biology, and evolutionary modelling. Swiss TPH supports capacity building through student supervision, technical mentorship, and maintenance of advanced research facilities alongside local technicians. NIMR strengthens national coordination and alignment with Tanzania’s research and public health priorities.

Research Technician Temesgen M Kebede, Transmission Zero, rearing malaria mosquitoes in the laboratory. Photograph: Transmission Zero
These partnerships go beyond science alone. Our programme brings international PhD students from Switzerland and elsewhere to work alongside Tanzanian researchers, fostering cross-cultural exchange and skills transfer. We are also investing in mathematical modelling capacity, with Tanzanian scientists collaborating with regional and international experts to predict gene drive mosquitoes’ behavior and assess the effectiveness of our technology in real-world settings. This modelling work is crucial for informing risk assessment, regulatory review, and long-term monitoring should the technology advance toward field trials.
Global partnerships help ensure that our innovation is developed safely, transparently, and in line with international best practices, while keeping leadership anchored in Tanzania, where malaria’s impact is most severe.
Working with local communities and national authorities
Our programme also places strong emphasis on cross-sectoral collaboration, recognizing that new technologies can only succeed if they are understood, governed, and ultimately accepted by those they are intended to serve.

Felista Tarimo, Ifakara Health Institute (IHI), taking part in a demonstration collecting mosquitoes. Photograph: Ifakara Health Institute
Stakeholder engagement is core to our work. Our team works closely with communities, policymakers, and civil society to share information about our work and answer their questions and concerns. Since 2024, field engagement activities in Ukerewe District, Mwanza Region, have supported transparency, trust-building, and two-way communication with communities living in malaria-endemic areas.
At the national level, we regularly convene stakeholders from government ministries, regulatory authorities, and research institutions. A recent meeting in Dar es Salaam for example, brought together the National Biosafety Committee, ministerial representatives, and representatives from organizations such as the International Union for Conservation of Nature (IUCN) to review progress and discuss ethical, environmental, and regulatory considerations.

Justina Mosha, National Institute for Medical Research, Tanzania (NIMR). Photograph: Ifakara Health Institute
Our approach has spanned the full spectrum of what it takes to beat this disease. Tanzania has invested in world-class research and is home to the Ifakara Health Institute, where our scientists are working at the frontier of new technologies, including gene drive—an innovative approach that aims to ensure mosquitoes can no longer transmit the malaria parasite. This is African science, conducted by African researchers, addressing an African challenge. – Tanzania’s President, H.E. Dr. Samia Suluhu Hassan, Speaking at the 39th African Union Summit
Our work at the Ifakara Health Institute under the Transmission Zero programme demonstrates what is possible when local leadership, global partnerships, and cross-sectoral collaboration converge. By anchoring cutting-edge science within malaria-endemic countries, strengthening national research capacity, and engaging openly with communities and governments, our programme offers a model for equitable innovation in global health. On this World Malaria Day, the message is clear: ending malaria is not only a scientific challenge, it is a collective endeavor.
